Liquid Biopsy for Lupus Nephritis – Urinary Biomarkers of Renal Pathology Activity and Chronicity
Lead: Michael Sheth
Team Members: Kamala Vanarsa, Anjani Marri, Ting Zhang
Collaborators: Ramesh Saxena, Michelle Petri, CC Mok
Project Summary:
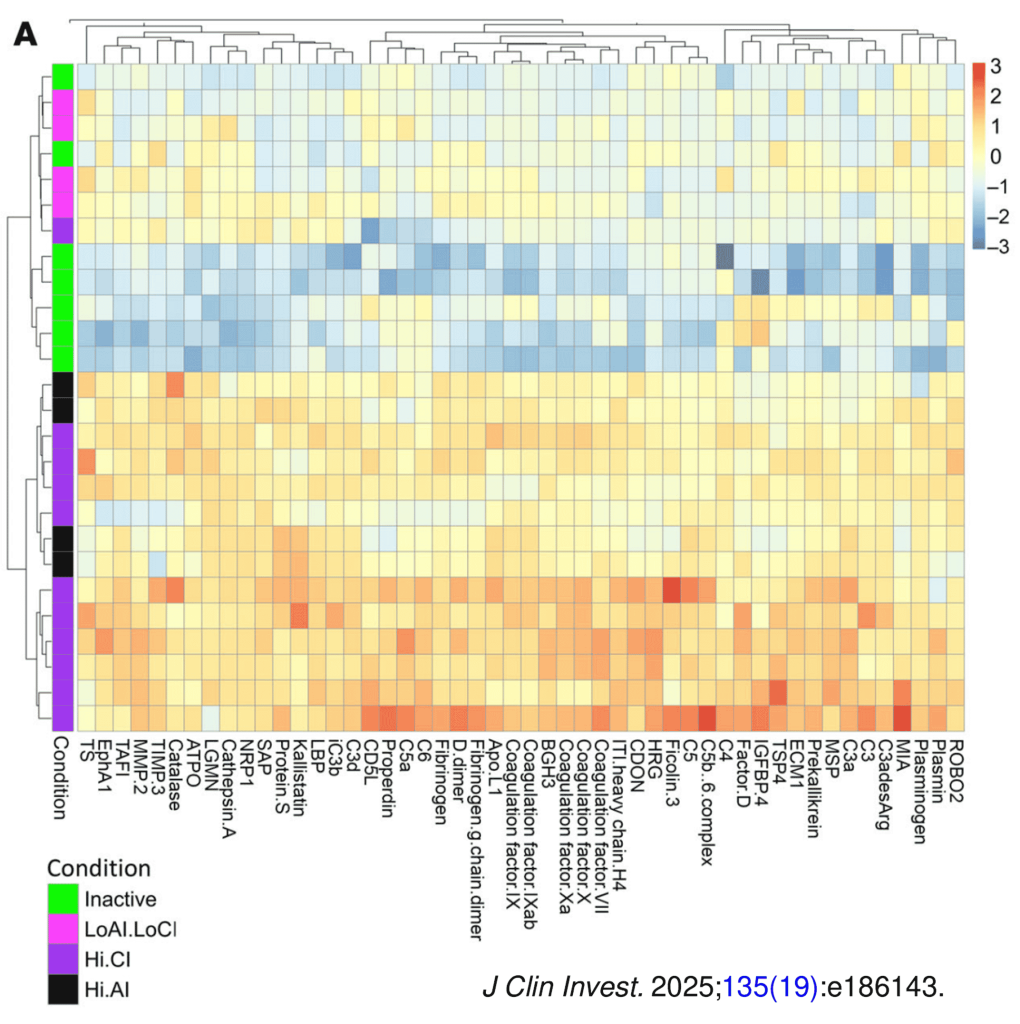
The current gold standard for assessing renal pathology in lupus nephritis (LN) is invasive and cannot be serially repeated. To assess if urine can serve as a liquid biopsy for underlying renal pathology, urine obtained from patients with LN at the time of renal biopsy were interrogated for 1,317 proteins, using an aptamer-based proteomic screen. Levels of 57 urine proteins were significantly elevated and correlated with pathology activity index (AI), notably endocapillary hypercellularity, fibrinoid necrosis, and cellular crescents. These included proteins pertaining to leukocyte/podocyte activation, neutrophil activation, endothelial activation, and markers of inflammation/anti-inflammation. In contrast, complement and coagulation cascade proteins, and proteins related to the extracellular matrix (ECM) emerged as the strongest urinary readouts of concurrent renal pathology chonicity index (CI), notably tubular atrophy and interstitial fibrosis. In vitro mechanistic studies revealed that complement proteins C3a and C5a increased the expression of profibrotic ECM proteins in macrophages and proximal tubule epithelial cells. Thus, carefully assembled panels of urinary proteins that are indicative of high renal pathology AI and/or CI may help monitor the status of renal pathology after therapy in patients with LN, in a noninvasive manner, without the need for repeat renal biopsies.
Building on the above completed report, the present study evaluates a targeted panel of inflammatory, coagulation-related, complement, and tissue remodeling proteins in an independent patient LN cohort, using ELISA.
What is already known in the field?
- Renal biopsy remains the reference standard for assessing LN activity and chronicity but is invasive and impractical for frequent monitoring.
- Proteomic studies have identified urinary proteins associated with renal inflammation and chronic damage in LN.
What is new?
- Independent ELISA-based validation of urinary biomarkers of renal pathology originally identified through proteomic screening.
- Systematic comparison of biomarker performance across clinical states, histologic classes, renal response status, and pathology indices.
Why this is important?
Renal pathology in lupus nephritis evolves dynamically, yet clinicians lack reliable non-invasive tools to track these changes over time. This project addresses a critical gap by identifying urinary biomarkers that reflect kidney-specific pathology. Establishing which urine biomarkers reliably align with histologic injury could reduce reliance on repeat biopsies, enable earlier detection of disease progression or incomplete treatment response, and support individualized patient management.